Michigan hospitals are still recovering from the pandemic, but a shortage of child adolescent psychiatrists has exacerbated the high demand for mental health care.
Abishek Bala is an assistant professor of psychiatry at Central Michigan University and a child and adolescent psychiatrist in Saginaw. He’s training medical residents and fellows to combat the shortage.
Bala, who manages an inpatient child and adolescent unit at HealthSource Saginaw, said the city has about five or six child and adolescent psychiatrists.
Children from all over the state are admitted to the unit, especially from Northern Michigan and the Thumb.
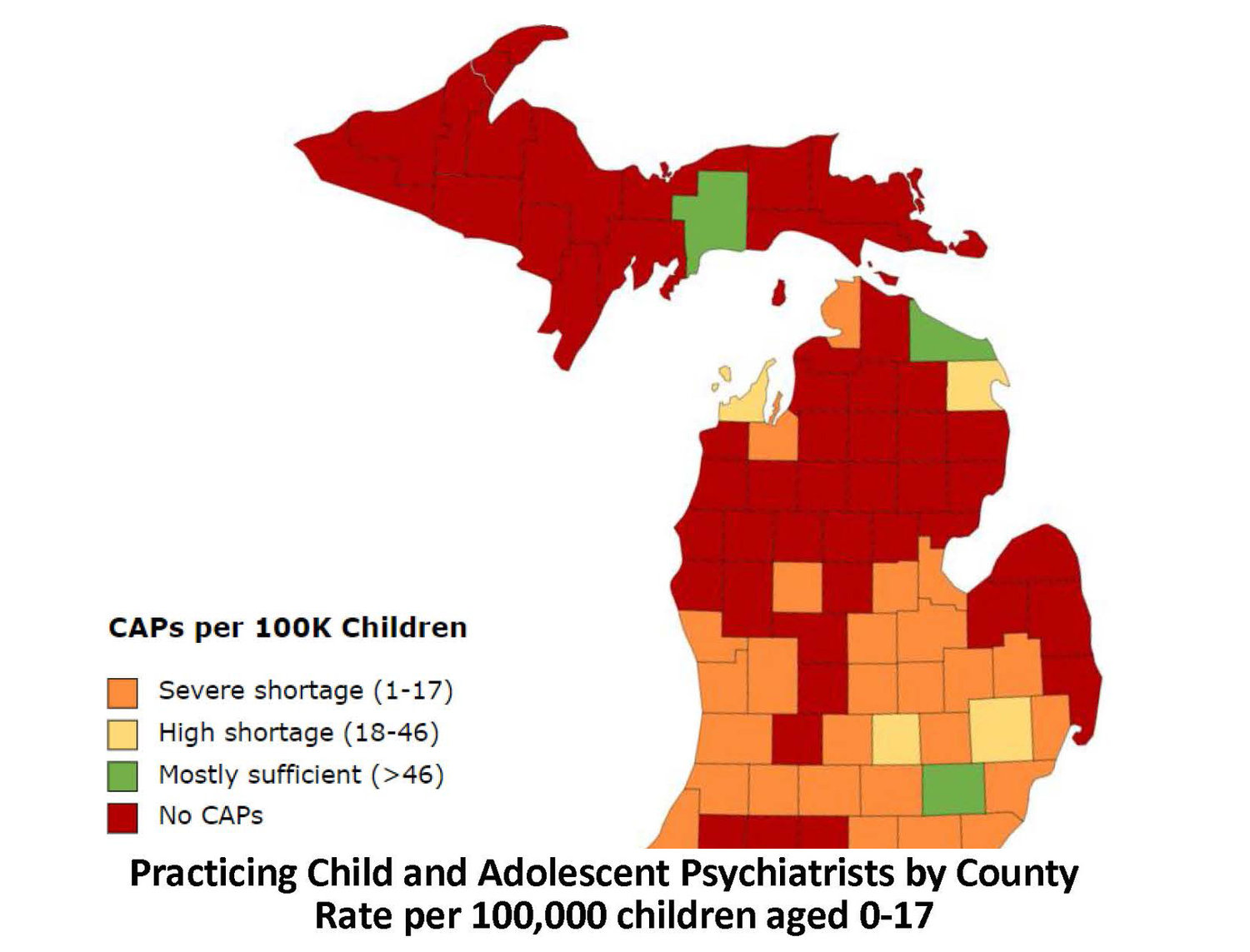
In many rural areas in Michigan, there is a severe shortage of child and adolescent psychiatrists, Bala said. There is only one practicing child psychiatrist in the Upper Peninsula according to the American Academy of Child and Adolescent Psychiatry.
“We have to ensure that we have solid mental health support for (these children), especially after they go through a crisis phase in their lives with a lot of stressors, a lot of trauma,” Bala said. “We have to return them to the community where we have no child psychiatrists, and we have limited community resources, which can be hard.”
General psychiatrists do treat children as patients, but Bala said it’s crucial to have specialized psychiatrists who can support their “developmental journey.”
“As a child psychiatrist, we have to essentially piece all of those very important aspects of their lives together while we formulate treatment,” Bala said. “Our job isn’t necessarily just to explore pharmacological options – we have to look into the holistic model.”
In 2021, the American Academy of Pediatrics, the American Academy of Child and Adolescent Psychiatry and the Children’s Hospital Association declared a national state of emergency in child and adolescent mental health.
Bala said there has been an increase in psychiatric and mental health illnesses like anxiety and depression over the past few years.
He said the goal of Central Michigan’s fellowship program is to address this growing need by adding to the mental health workforce and collaborating with the community.
“I think we’re on the right track from what we’ve done so far, but we have quite a long journey yet,” Bala said. “That requires a lot of support, a lot of collaboration. But I’m optimistic.”
The Northern Lakes Community Mental Health Authority in Traverse City serves residents of Grand Traverse, Leelanau, Crawford, Roscommon, Missaukee and Wexford counties.
Medical director Curtis Cummins said the authority employs only one child and adolescent psychiatrist and is in the process of hiring another.
Cummins said he thinks that will be enough to meet the needs of the authority’s counties. He said other entities without access to child and adolescent psychiatrists may have pediatricians or primary care providers provide mental health support.
“We are fortunate enough that we are able to provide those services,” Cummins said. “We don’t need to look at people that are not trained.”
He said a lack of job openings may be contributing to the shortage of child and adolescent psychiatrists.
Cummins said smaller community mental health centers might not see a high need for a specialized child psychiatrist.
“Sometimes in rural America, it’s hard for them to land and search for that employment,” Cummins said. “I know a number of child and adolescent psychiatrists in Northern Michigan that serve adults or they’re in administrative roles.”
Laura Appel, the executive vice president of government relations and public policy of the Michigan Health and Hospital Association, said the association hopes to bring more psychologists into the state and improve the safety of hospital emergency departments.
People without access to psychiatric care might use only emergency services, “not because we want a psych ward inside an emergency department, but because we actually have that going on,” Appel said. “We have to meet the responsibility of covering the cost of that.”






Comments
No comments on this item Please log in to comment by clicking here